Neutrophils are the most common type of white blood cell, making up 50–70% of all circulating leukocytes in the human body1 2. They serve as the body's first line of defense against infections by rapidly responding to invading pathogens and tissue damage3 . These cells not only fight infections but also help regulate inflammation and promote tissue repair, playing a vital role in maintaining immune system balance1 45.
Neutrophil Functions and Actions
Neutrophils, also known as polymorphonuclear cells (PMNs), are a major subset of white blood cells essential for innate immunity1 6. They are the first responders to infection or injury, migrating quickly to affected tissues in response to chemotactic signals such as chemokines and cytokines1 27. Once at the site, neutrophils eliminate pathogens through several mechanisms:
- Phagocytosis: Neutrophils engulf and digest bacteria and other microorganisms1 89.
- Degranulation: They release cytotoxic granules containing enzymes that destroy pathogens1 8.
- Neutrophil Extracellular Traps (NETs): Neutrophils release sticky webs of DNA and proteins that trap and kill microbes1 410.
Beyond these classical antimicrobial functions, neutrophils also influence adaptive immunity by interacting with T and B cells and can act as antigen-presenting cells (APCs) under certain conditions11 . They modulate immune responses by releasing cytokines and chemokines that recruit and activate other immune cells12 7. Neutrophils also contribute to tissue repair and the resolution of inflammation, highlighting their functional diversity1 45.
Neutrophils are produced continuously in the bone marrow, where they mature before entering the bloodstream1 2. Mature neutrophils circulate in the blood for 1–5 days before migrating into tissues or undergoing programmed cell death (apoptosis) 113. The body produces approximately 100 billion neutrophils daily to maintain this critical defense system3 12.
“Neutrophils, the most abundant type of granulocyte, are widely recognized as one of the pivotal contributors to the acute inflammatory response. Initially, neutrophils were considered the mobile infantry of the innate immune system, tasked with the immediate response to invading pathogens.”
— Kraus & Gruber14
Measuring Neutrophil Levels
Neutrophil levels in the blood are measured using a complete blood count (CBC), a routine laboratory test that evaluates different types of blood cells15 16. The CBC provides a detailed overview of white blood cells, including neutrophils, lymphocytes, and monocytes15 16. From the CBC, the absolute neutrophil count (ANC) is calculated, indicating the number of neutrophils per microliter (µL) of blood15 16.
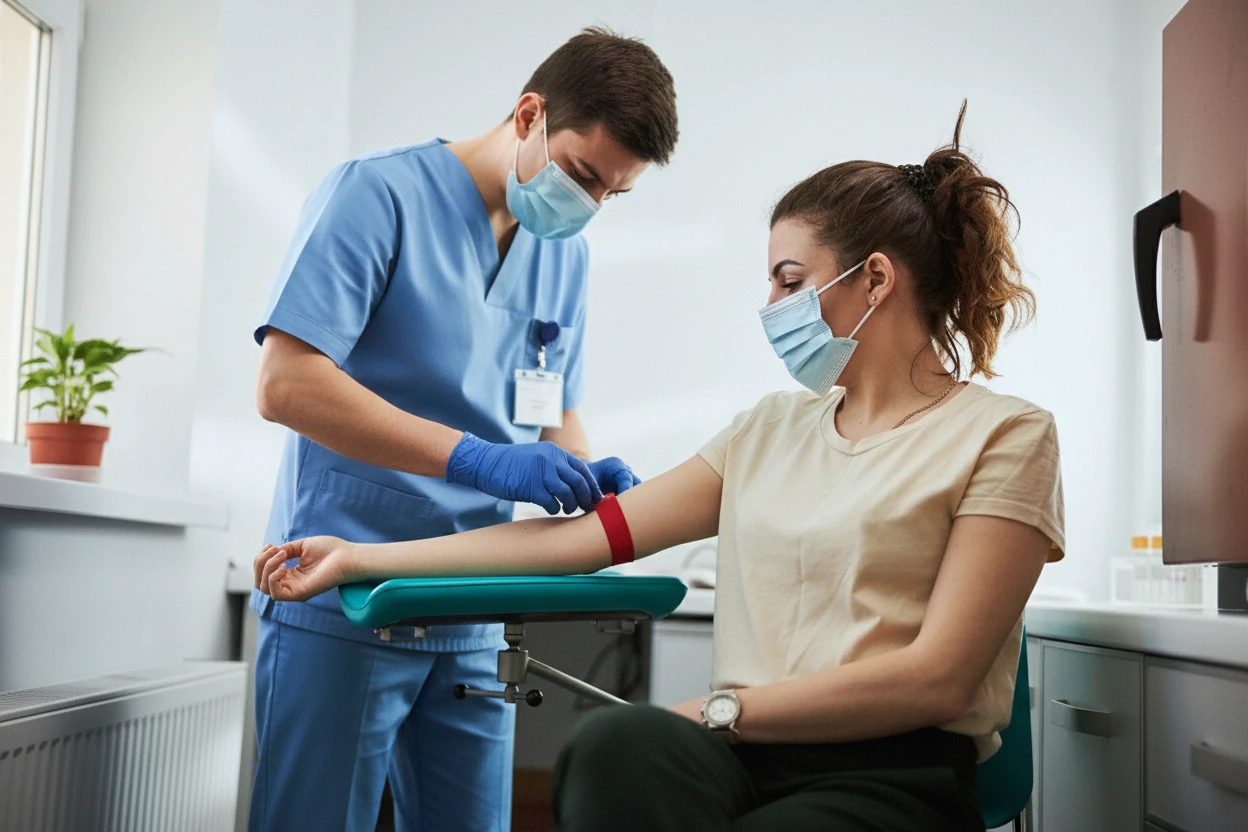
Blood samples for this test are typically obtained through venipuncture15 16. Reference ranges for neutrophil counts vary by age, with children generally having higher counts than adults due to immune system development15 16. In healthy adults, the normal neutrophil count ranges from approximately 2,500 to 7,000 cells/µL15 165.
Monitoring neutrophil levels is crucial for diagnosing and managing infections, hematologic disorders, cancer, and inflammatory diseases15 16. Changes in neutrophil counts can indicate immune system activation or suppression and guide further clinical evaluation15 16.
Low Neutrophil Count Causes
A low neutrophil count, known as neutropenia, is defined as an ANC below 1,500 cells/µL in adults15 165. Neutropenia increases the risk of infections because the body's first line of defense is weakened15 16. The severity of neutropenia is classified as:
- Mild: 1,000–1,500 cells/µL
- Moderate: 500–1,000 cells/µL
- Severe: Less than 500 cells/µL15 16
Common causes of neutropenia include:
- Bone marrow disorders: Conditions like aplastic anemia impair neutrophil production15 16.
- Hematologic malignancies: Leukemia and lymphoma disrupt normal bone marrow function15 16.
- Autoimmune diseases: Diseases such as systemic lupus erythematosus (SLE) and rheumatoid arthritis cause immune-mediated destruction of neutrophils15 1617.
- Infections: Severe or chronic infections can deplete neutrophil reserves5 .
- Medications: Antibiotics, chemotherapeutic agents, and radiation therapy can suppress bone marrow activity leading to neutropenia15 165.
Neutropenia can be transient or chronic, and its presence often requires careful monitoring to prevent life-threatening infections15 165.
High Neutrophil Count Implications
An elevated neutrophil count, or neutrophilia, is defined as an ANC above 7,500 cells/µL in adults15 165. Neutrophilia commonly indicates an ongoing infection or inflammatory process but can also result from stress, trauma, or medication effects15 16.
“In the past 10 years or so, there has been increasing evidence that cancer cells produce various factors that induce neutrophils to form NETs (the sticky webs) and that these NETs promote metastasis.”
— Honami Naora, MD Anderson Cancer Center18
Conditions associated with neutrophilia include:
- Acute bacterial infections: Neutrophils increase rapidly to combat pathogens15 165.
- Inflammatory diseases: Chronic inflammation from conditions like rheumatoid arthritis or inflammatory bowel disease can raise neutrophil levels15 165.
- Stress responses: Physical or emotional stress can trigger neutrophilia15 16.
- Tissue injury: Burns and surgical trauma induce neutrophil recruitment as part of the acute phase response15 16.
- Medications: Corticosteroids and epinephrine can cause elevated neutrophil counts15 16.
Persistent neutrophilia may warrant further investigation to identify underlying causes and assess for potential complications15 16.
“We found that NETs cause other types of immune cells in the omentum to become less effective in defending against cancer cells, making the metastasis more likely to occur.”
— Honami Naora, MD Anderson Cancer Center18
Treating Abnormal Neutrophil Levels
Treatment of abnormal neutrophil counts depends on the underlying cause and severity of the condition. Management aims to restore immune balance and prevent complications such as infections or excessive inflammation.
Treatment for Low Neutrophils
For neutropenia, especially when severe, treatment options include:
- Antibiotics: Used prophylactically or therapeutically to prevent or treat infections15 16.
- Granulocyte colony-stimulating factor (G-CSF): A growth factor that stimulates neutrophil production and enhances their function15 16.
- Discontinuation or substitution of causative medications: To prevent further bone marrow suppression15 16.
- Hospitalization and supportive care: For severe cases to monitor and manage infection risk15 16.
Identifying and treating the underlying cause, such as autoimmune disease or bone marrow disorder, is essential for effective management15 16.
Treatment for High Neutrophils
Managing neutrophilia focuses on addressing the primary condition causing the elevated count:
- Treat infections or inflammation: Appropriate antimicrobial or anti-inflammatory therapies reduce neutrophil activation15 16.
- Medication review: Adjust or discontinue drugs that may cause neutrophilia15 16.
- Monitoring: Persistent neutrophilia requires evaluation for chronic diseases or malignancies15 16.
Controlling the underlying disease helps normalize neutrophil levels and prevents complications related to excessive inflammation15 16.
Questions for Your Healthcare Provider
If you have abnormal neutrophil counts, consider discussing the following with your healthcare provider:
- What might be causing my low or high neutrophil count? 1516
- Do I need further tests to diagnose the underlying condition? 1516
- What treatments are available for my neutrophil count abnormality? 1516
- How can I reduce my risk of infections if I have neutropenia? 1516
- Should I adjust any medications that might affect my neutrophil levels? 1516
- How often should my neutrophil counts be monitored? 1516
- What lifestyle changes can support my immune health? 1516
Open communication about symptoms, medications, and lifestyle factors can help your provider tailor the best care plan for you15 16.
Key Takeaways
- Neutrophils are the most abundant white blood cells and serve as the first line of defense against infections and tissue injury1 23.
- They eliminate pathogens through phagocytosis, degranulation, and NET formation, while also regulating inflammation and adaptive immunity1 411.
- Normal neutrophil counts in adults range from 2,500 to 7,000 cells/µL; values outside this range may indicate health issues15 165.
- Low neutrophil counts (neutropenia) increase infection risk and may result from bone marrow disorders, autoimmune diseases, infections, or medications15 16.
- High neutrophil counts (neutrophilia) often reflect infection, inflammation, stress, or medication effects and require evaluation of the underlying cause15 16.
- Treatment focuses on addressing the root cause, preventing infections in neutropenia, and controlling inflammation in neutrophilia15 16.