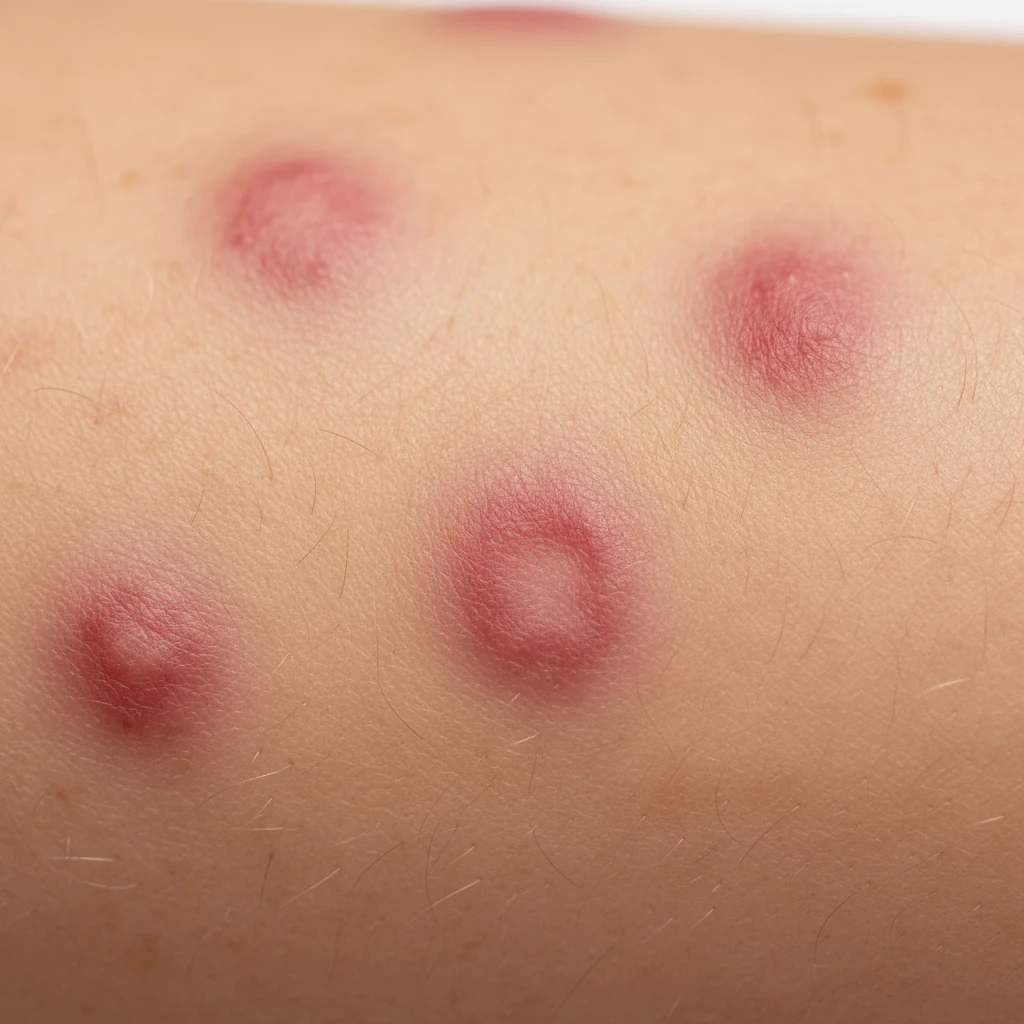
Stress can cause visible changes in the skin, including rashes and hives, which affect many people especially during periods of high psychological distress1 . These skin reactions often appear as raised, red, itchy bumps that may burn or tingle and can occur anywhere on the body2 . Stress not only triggers new skin outbreaks but can also worsen existing conditions like eczema, psoriasis, and acne3 4. Understanding the symptoms, causes, and treatment options for stress-related skin issues is essential for effective management and relief.
Stress Rash Symptoms
Stress rashes typically manifest as raised, discolored bumps known as hives or urticaria, commonly appearing on the face, chest, neck, or arms but potentially anywhere on the body2 . These rashes may be itchy, burn, or tingle and often feel warm to the touch2 . The rash can range from small dots to large welts, sometimes forming clusters that are sensitive and swollen3 . Stress causes the body to release chemicals that trigger inflammation and increase skin sensitivity, which can lead to these flare-ups3 .
Stress rashes may be acute, clearing up within six weeks, or chronic if they persist longer5 . Most stress-induced rashes resolve on their own within a few days, but some can last up to six weeks or more3 . Scratching the rash can worsen symptoms and increase the risk of secondary infection3 . Stress rashes may also cause symptoms such as blisters, pain, raw skin, or irritation in severe cases6 .
- Raised red bumps or welts that may itch or burn2
- Warm, swollen, or blotchy skin areas2
- Tingling or stinging sensations when touched2
- Rash often appearing on face, neck, chest, or arms but can occur anywhere3
- Possible blisters, peeling, or raw skin in severe cases6
💡 Did You Know?
Stress can cause a rash or hives, and it can also worsen existing skin conditions. Treatment options may include cold compress, antihistamines, steroids, and more5 .
When you're feeling stress, your body releases chemicals that can cause inflammation and make your skin even more sensitive.3
Stress Hives (Urticaria)
Hives, medically known as urticaria, are raised, itchy, erythematous (red) wheals that can appear anywhere on the skin7 . Stress is a recognized trigger for chronic spontaneous urticaria (CSU), which can both start and worsen hives in some patients7 8. The exact mechanism is not fully understood, but stress likely influences mast cell activity, leading to histamine release that causes the characteristic swelling and itch7 .
Individual hives usually last less than 24 hours, but new lesions may appear as older ones fade, causing a fluctuating rash pattern7 . Hives may be accompanied by itching, burning, or stinging sensations7 . Physical triggers such as pressure, temperature changes, and infections can also provoke histamine release and urticaria7 . Temperature extremes and mechanical pressure can induce physical urticarias, including dermatographism, where the skin becomes raised and inflamed after scratching or rubbing7 .
Stress activates the hypothalamic-pituitary-adrenal (HPA) axis, leading to cortisol release that modulates immune responses and may trigger mast cell degranulation9 10. This neuroimmune interaction contributes to skin inflammation and hives during stressful periods9 10.
- Itchy, raised red welts on the skin that may burn or sting7
- Lesions typically resolve within 24 hours but new ones can form7
- Stress can trigger or worsen chronic spontaneous urticaria7 8
- Physical triggers like heat, cold, or pressure may also provoke hives7
- Mast cells release histamine, causing swelling and itching7 11
“Stress hives are a real physical manifestation of stress. The body's response to stress can include release of histamine, which can cause hives similar to an allergic reaction.”
— Brian Myers, Cleveland Clinic12
Treating Stress-Related Rashes
Most stress-induced rashes and hives are mild and can be managed at home with simple remedies1 . Over-the-counter (OTC) antihistamines such as cetirizine, loratadine, or diphenhydramine can reduce itching and swelling by blocking histamine effects2 6. Cooling the skin with cold compresses, lukewarm showers, or oatmeal baths can relieve discomfort and reduce inflammation2 3. Avoiding hot showers, tight clothing, and irritants like fragrances helps prevent worsening symptoms2 .
For persistent or severe cases, doctors may prescribe stronger antihistamines, corticosteroids, or topical cortisone creams to reduce inflammation and promote healing3 6. In chronic urticaria unresponsive to first-line treatments, advanced therapies such as omalizumab (an anti-IgE monoclonal antibody) or immunosuppressants like cyclosporine may be considered under specialist care7 . Stress management techniques including mindfulness meditation, yoga, exercise, and therapy are recommended adjuncts to reduce flare-ups, although evidence for their direct effect on skin symptoms is limited9 .
- Non-sedating antihistamines (cetirizine, loratadine) as first-line therapy7
- Cold compresses and oatmeal baths to soothe itching and inflammation2 3
- Avoidance of physical triggers such as heat, pressure, and irritants7 2
- Prescription corticosteroids or stronger antihistamines for severe cases7 3
- Advanced immunomodulators like omalizumab or cyclosporine for chronic, refractory urticaria7
- Stress reduction techniques including mindfulness, exercise, and therapy9
“If your rash doesn't respond to home treatment, we may prescribe a stronger antihistamine or a cortisone cream to knock down the inflammation and help your skin heal.”
— Erin Lester, Scripps Coastal Medical Center3
How Stress Triggers Skin Reactions
Stress activates the hypothalamic-pituitary-adrenal (HPA) axis and the sympathetic nervous system, leading to the release of hormones such as cortisol, catecholamines, and neuropeptides9 10. These stress hormones modulate immune cell activity in the skin, particularly mast cells, which release histamine and other inflammatory mediators that cause itching and swelling7 910.
The skin’s response to stress involves complex neuroendocrine and immune interactions as well as impaired skin barrier function, which can exacerbate inflammation and sensitivity9 10. Chronic stress is linked to higher rates of skin symptoms such as itching, rash, and hair loss, especially in populations under high psychological stress like medical students13 . Inflammatory skin diseases such as atopic dermatitis and psoriasis are particularly sensitive to stress, with flares often occurring during periods of increased psychological distress9 10.
Stress can also increase the production of immune cells, potentially triggering autoimmune reactions that worsen skin conditions2 . The precise mechanisms remain incompletely understood but involve multifaceted interactions between nerves, immune cells, and skin barrier integrity9 10.
- Activation of the HPA axis and sympathetic nervous system releasing cortisol and catecholamines9 10
- Modulation of mast cells leading to histamine release and skin inflammation7 11
- Impaired skin barrier function increasing sensitivity and inflammation9 10
- Increased immune cell production potentially triggering autoimmune skin reactions2
- Stress-induced flares in chronic inflammatory skin diseases like eczema and psoriasis9 1013
Stress triggers chemical changes that cause inflammation and skin sensitivity, leading to rashes and hives. Managing stress can help reduce these skin flare-ups and improve overall skin health1 3.
When to See a Doctor
Most stress-related rashes and hives resolve on their own or with OTC treatments, but medical evaluation is important if symptoms are persistent, severe, or recurrent7 . Seek medical attention if hives cover large areas, are accompanied by skin peeling, blisters, fever, or pain, as these may indicate a more serious condition5 . Persistent urticaria lasting longer than six weeks is considered chronic and requires specialist assessment7 .
Emergency care is necessary if hives are associated with swelling of the mouth, throat, or difficulty breathing, which may signal anaphylaxis6 . Secondary infection of skin lesions due to scratching may require antimicrobial therapy7 . Referral to a dermatologist or allergist is recommended for cases unresponsive to first-line treatments or when advanced therapies are needed7 .
- Rash or hives lasting longer than a few days or recurring frequently5 7
- Extensive rash with blistering, peeling, fever, or pain5
- Signs of infection such as redness, warmth, or pus7
- Difficulty breathing, swelling of face or throat, or other allergic symptoms6
- Chronic urticaria persisting beyond six weeks7
- Lack of response to OTC antihistamines or home remedies7
Summary
Stress-induced skin reactions such as rashes and hives are common and result from complex neuroimmune and hormonal changes triggered by psychological stress7 910. These skin symptoms often appear as itchy, raised, red bumps that may burn or tingle and can affect any part of the body2 3. Stress not only causes new skin outbreaks but can also worsen existing inflammatory skin conditions like eczema and psoriasis9 1013.
Most stress rashes and hives are mild and respond well to home treatments including cold compresses and OTC antihistamines2 5. For persistent or severe cases, medical evaluation and prescription therapies such as corticosteroids or immunomodulators may be necessary3 7. Stress management through mindfulness, exercise, and relaxation techniques is a valuable adjunct to reduce flare-ups and improve skin health1 9.
Early recognition and treatment of stress-related skin conditions can prevent complications and improve quality of life. If symptoms persist or worsen, consulting a healthcare professional is essential for tailored care and advanced treatment options7 .
- Stress activates hormonal and immune pathways that cause skin inflammation and sensitivity9 10
- Stress rashes often present as itchy, red, raised bumps or hives that may burn or tingle2 3
- Most cases improve with cold compresses and OTC antihistamines; severe cases may need prescription medications3 7
- Managing stress through relaxation techniques can help reduce skin flare-ups1 9
- Seek medical care if rashes last more than a few days, worsen, or are accompanied by systemic symptoms6 7