Glaucoma is a leading cause of irreversible vision loss worldwide, affecting millions of people and often progressing silently without early symptoms1 . This group of eye diseases damages the optic nerve, primarily due to increased intraocular pressure (IOP), which can lead to permanent vision loss if untreated2 . Early diagnosis and consistent management are essential to slow or prevent vision loss and maintain quality of life3 .
Medication Treatments for Glaucoma
Medical management is frequently the first choice in most cases of glaucoma and remains the usual first-line therapy3 4. The primary goal of pharmacotherapy is to lower intraocular pressure, the only proven intervention to prevent glaucomatous optic nerve damage5 . Medications achieve this by either decreasing the production of aqueous humor (the fluid inside the eye) or increasing its outflow3 .
Prostaglandin analogs are considered the most efficacious topical agents and are typically the first-line medications due to their high efficacy and favorable safety profile6 7. They work by increasing uveoscleral outflow, which helps reduce eye pressure by facilitating fluid drainage through alternative pathways6 7. Other classes of medications include:
- Beta-blockers: Reduce aqueous humor production, lowering eye pressure6 7.
- Alpha-adrenergic agonists: Both decrease fluid production and increase outflow; brimonidine is a commonly used alpha-2 agonist6 7.
- Carbonic anhydrase inhibitors: Decrease aqueous humor production6 7.
- Cholinergic (miotic) agents: Stimulate the ciliary muscle to open the trabecular meshwork, enhancing outflow6 .
- Rho kinase inhibitors: Such as netarsudil, enhance trabecular outflow by suppressing enzymes that increase fluid resistance6 7.
Combination eye drops that include two active agents can provide greater pressure reduction with fewer drops, improving adherence7 . However, side effects may occur, including local irritation, changes in eye color, or systemic effects like headaches or changes in heart rate, due to absorption of medication into the bloodstream7 8.
Adherence to glaucoma medications is critical, as failure to use prescribed eye drops daily can increase the risk of vision loss8 . Regular monitoring and adjustment of therapy are essential to achieve the recommended IOP reduction of 20% to 50% from baseline, tailored to the extent of optic nerve damage and disease progression3 9.
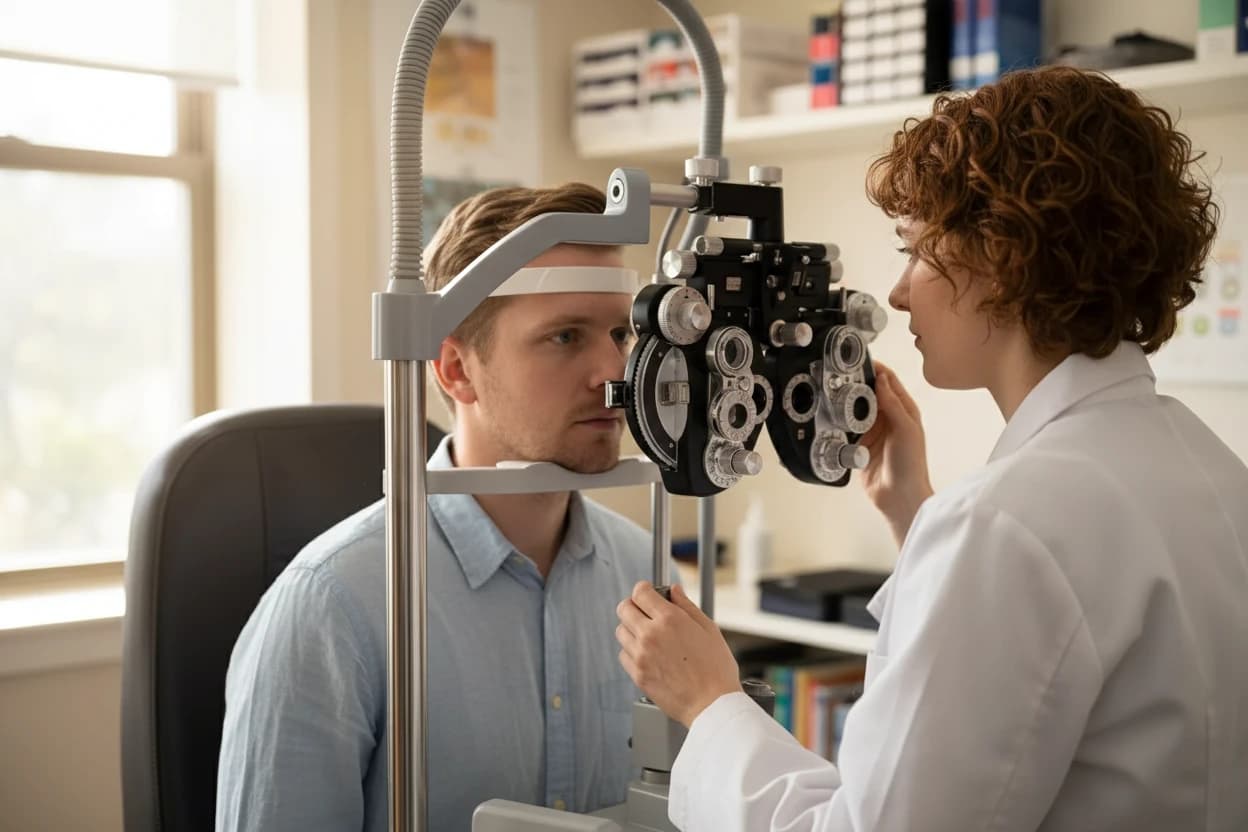
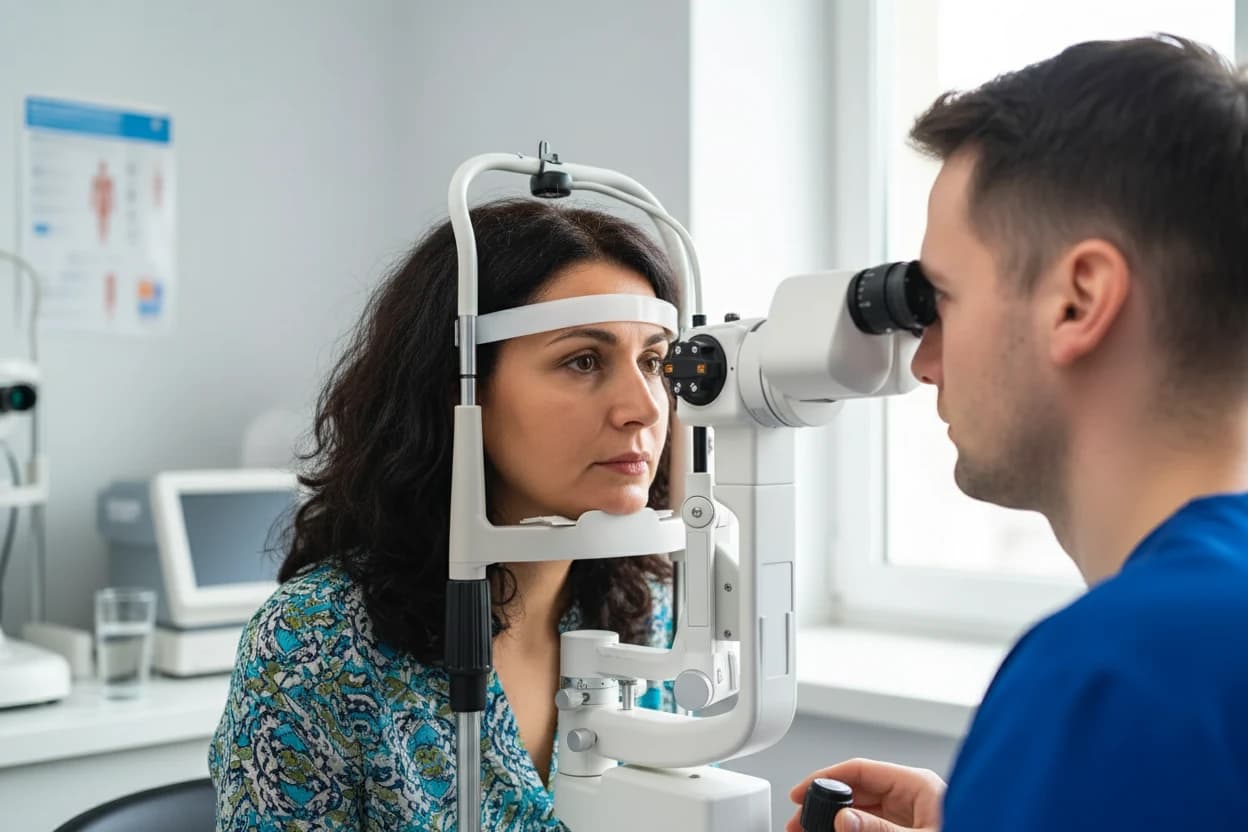
An eye care professional will review your medical history and perform tests such as tonometry (measuring eye pressure), visual field testing, and gonioscopy (examining the drainage angle) to diagnose and monitor glaucoma10 .
Laser Therapy for Glaucoma
Selective laser trabeculoplasty (SLT) is a non-invasive laser treatment increasingly used as a first-line or adjunctive therapy for open-angle glaucoma11 12. SLT works by targeting specific cells in the trabecular meshwork, improving aqueous humor drainage and thereby lowering intraocular pressure11 13.
SLT is typically performed in an outpatient clinic setting under topical anesthesia, making it a convenient option for many patients11 13. The procedure can be done on one or both eyes depending on clinical judgment11 . Most patients experience only transient visual symptoms such as mild irritation or blurry vision immediately after treatment and can resume normal activities within 24 hours11 12.
While SLT is as effective as topical medications in lowering IOP and has fewer side effects, its effect may diminish over time, necessitating repeat treatments or additional therapies4 1112. Some patients may still require adjunctive medical therapy after SLT to maintain target IOP levels11 .
Laser therapy options vary depending on glaucoma type and severity. For example, laser peripheral iridotomy (LPI) is used in angle-closure glaucoma to create a small hole in the iris, allowing fluid to flow and relieving pressure13 . Laser cyclophotocoagulation targets the ciliary body to reduce fluid production and is typically reserved for advanced cases13 .
Surgical Procedures for Glaucoma
Surgery is generally indicated when maximal medical and laser therapies fail to control intraocular pressure adequately14 . The goal of glaucoma surgery is to create new pathways for aqueous humor drainage or reduce fluid production to prevent further optic nerve damage and vision loss4 .
Trabeculectomy
Trabeculectomy is the most common surgical procedure for open-angle glaucoma4 . It involves creating a new drainage pathway by making an opening in the sclera (the white of the eye) to allow aqueous humor to bypass the blocked trabecular meshwork and drain into a filtering bleb under the conjunctiva4 .
This procedure is usually performed under local anesthesia on one eye at a time and typically lasts less than an hour4 . It is an outpatient surgery, but patients require transportation home due to temporary vision changes and sedation4 . Recovery takes several weeks, during which anti-inflammatory and antibiotic eye drops are used to prevent infection and control inflammation4 .
Trabeculectomy can provide long-term intraocular pressure control, but some patients may require additional procedures or medications to maintain target IOP4 .
Glaucoma Implant Surgery
Glaucoma drainage devices, or tube shunts, are used in more complex cases, such as neovascular glaucoma or congenital glaucoma, where trabeculectomy may be less effective4 . These implants consist of a small tube inserted into the eye to drain excess aqueous humor to an external reservoir, lowering eye pressure4 .
Glaucoma implant surgery typically lasts 1–2 hours and is performed under local anesthesia4 . Like trabeculectomy, it is an outpatient procedure requiring postoperative care with anti-inflammatory and antibiotic drops4 . Implants can provide long-term pressure control but may also require additional interventions over time4 .
Minimally Invasive Glaucoma Surgery (MIGS)
MIGS procedures are gaining popularity due to their improved safety profiles and shorter recovery times compared to traditional surgeries4 15. These techniques aim to enhance aqueous outflow with less tissue disruption and fewer complications15 .
MIGS can be performed alone or combined with cataract surgery and are typically considered for mild-to-moderate open-angle glaucoma15 . They offer a faster recovery and reduced postoperative care, making them an attractive option for many patients15 .
| Surgical Procedure | Duration | Anesthesia | Recovery Time | Indications |
|---|---|---|---|---|
| Trabeculectomy | < 1 hour | Local | Several weeks | Open-angle glaucoma |
| Glaucoma Implant Surgery | 1–2 hours | Local | Several weeks | Complex glaucoma (e.g., neovascular) |
| Minimally Invasive Glaucoma Surgery (MIGS) | Varies (short) | Local | Shorter recovery | Mild-to-moderate open-angle glaucoma |
| Sources: 41415 | ||||
Medicated Eye Implants
Sustained-release drug delivery systems are emerging as a new treatment modality designed to improve medication adherence and provide continuous intraocular pressure control16 . These implants release glaucoma medications over several months, reducing the need for daily eye drops and improving compliance16 .
Examples include:
- Durysta: A biodegradable implant that releases bimatoprost over several months and does not require removal after drug release16 .
- iDose TR: A sustained-release reservoir implanted in the anterior chamber of the eye, providing continuous drug delivery16 .
These implants offer the advantage of steady medication levels, potentially improving treatment outcomes and reducing the burden of daily dosing16 . Sustained-release therapies are expected to play a larger role in glaucoma management in the future as technology advances16 .
Sustained-release implants like Durysta and iDose TR can help patients who struggle with daily eye drop regimens by providing continuous medication delivery, improving adherence and potentially better controlling intraocular pressure over time16 .
Living With Glaucoma Management
Glaucoma requires lifelong adherence to treatment and regular monitoring to prevent progression and vision loss3 . Patients must follow prescribed medication regimens carefully and attend routine eye exams to adjust therapy as needed3 .
Lifestyle factors can also influence glaucoma progression. Maintaining a healthy weight, controlling blood pressure, avoiding smoking, and engaging in regular physical activity may help reduce risk and support eye health3 . Systemic conditions such as hypertension and obesity have been linked to glaucoma risk and progression3 .
Regular intraocular pressure monitoring and visual field testing are crucial for detecting disease progression early and modifying treatment plans accordingly3 . Patients should be educated on the importance of adherence and lifestyle modifications to optimize outcomes.
Glaucoma Treatment Summary
Glaucoma is a chronic, progressive optic neuropathy that can lead to irreversible vision loss if untreated3 . The mainstay of treatment is lowering intraocular pressure through medications, laser therapy, or surgery3 4. Early detection and regular follow-up are essential for preserving vision and quality of life3 .
Untreated glaucoma can lead to loss of central vision and eventual blindness, but with proper treatment, progression can often be slowed or halted3 .
Treatment options include:
- Medications: First-line therapy using prostaglandin analogs, beta-blockers, alpha-agonists, carbonic anhydrase inhibitors, and newer agents like rho kinase inhibitors3 67.
- Laser therapy: Selective laser trabeculoplasty and laser peripheral iridotomy offer effective, minimally invasive options to lower eye pressure11 1213.
- Surgery: Trabeculectomy, glaucoma drainage devices, and minimally invasive glaucoma surgeries provide options when medical and laser treatments are insufficient4 14.
- Medicated implants: Sustained-release devices improve adherence and provide continuous drug delivery16 .
Successful glaucoma management depends on individualized treatment plans, patient adherence, and regular monitoring to prevent vision loss3 18.