Open-angle glaucoma is the most common form of glaucoma worldwide, affecting over 70 million people and representing a leading cause of irreversible blindness1 2. This eye disease progresses silently, often without symptoms until significant vision loss has occurred, making early detection and treatment critical to preserving sight3 4. The condition damages the optic nerve, primarily due to increased pressure inside the eye, and typically worsens over years if left untreated2 3.
Open-Angle Glaucoma Symptoms
Open-angle glaucoma usually begins without noticeable symptoms, making it difficult for patients to recognize the disease early5 . The condition is slowly progressive and can take years before symptoms become apparent6 . Early damage to the optic nerve can be compensated by eye movements, further delaying symptom recognition7 . Typically, both eyes are affected, although the severity may differ between them2 .
The hallmark of early open-angle glaucoma is loss of peripheral (side) vision, while central vision remains intact until the disease reaches advanced stages2 7. This peripheral vision loss often manifests as a narrowing of the visual field, commonly described as tunnel vision2 . As glaucoma progresses, patients may develop visual field defects such as scotomas—blind spots within the visual field8 . In advanced stages, visual acuity may decrease, and untreated glaucoma can ultimately lead to irreversible blindness2 68.
- Early glaucoma usually has no symptoms and patients are often unaware of the problem5 .
- Peripheral vision loss is the first sign, with central vision preserved until late stages2 7.
- Visual field narrowing is often described as tunnel vision2 .
- Visual field defects like scotomas appear as the disease progresses8 .
- If untreated, glaucoma can cause permanent blindness2 .
Open-angle glaucoma is often called the silent thief of sight because it causes gradual vision loss without warning signs until significant damage has occurred3 9.
Open-Angle Glaucoma Causes
Open-angle glaucoma is a chronic, progressive optic neuropathy characterized by damage to the optic nerve due to elevated intraocular pressure (IOP) 1011. The optic nerve is composed of retinal ganglion cells that transmit visual signals from the eye to the brain. In glaucoma, these cells progressively die, leading to optic nerve damage and vision loss2 7.
The eye contains a clear fluid called aqueous humor, which fills the anterior chamber and is continuously produced and drained to maintain normal eye pressure2 12. The trabecular meshwork, located at the angle where the iris meets the cornea, is the primary drainage pathway for aqueous humor12 . In open-angle glaucoma, the drainage angle appears open, but resistance within the trabecular meshwork reduces fluid outflow, causing increased IOP12 3. Elevated IOP damages the optic nerve by straining the lamina cribrosa, the supportive structure of the optic nerve head, leading to axonal injury and cell death13 .
Risk Factors
Several risk factors increase the likelihood of developing open-angle glaucoma:
- Older age is a significant risk factor, with prevalence increasing after age 40 and especially over 6014 1015.
- People of African descent have a higher prevalence and risk, often developing glaucoma earlier and with more severe vision loss5 315.
- Family history of glaucoma increases risk substantially10 15.
- Elevated intraocular pressure is the major modifiable risk factor12 4.
- Other factors include thin central corneas, high myopia or hyperopia, and certain medical conditions like diabetes and hypertension15 .
Glaucoma can occur even with normal eye pressure, a condition known as normal-tension glaucoma, possibly due to optic nerve sensitivity or reduced blood flow16 3.
Diagnosing Open-Angle Glaucoma
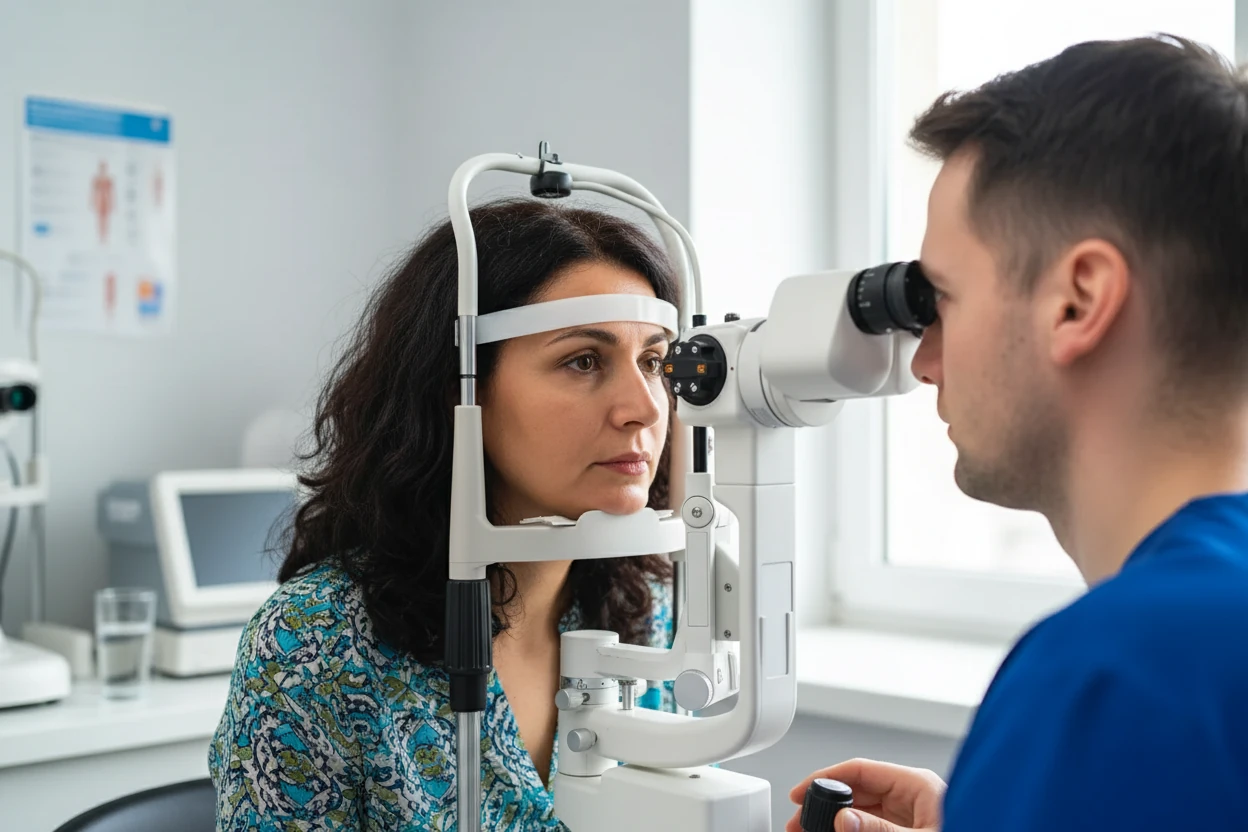
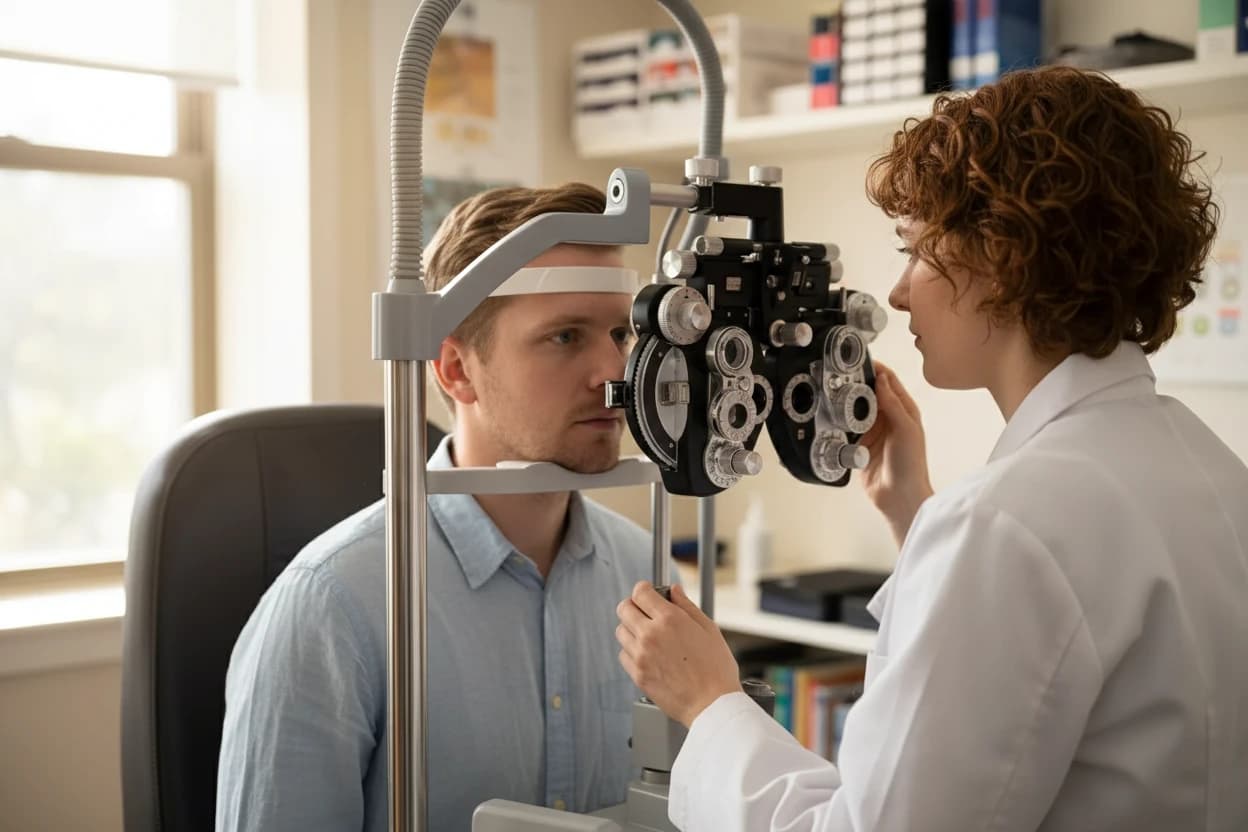
Diagnosing open-angle glaucoma involves a comprehensive eye examination to detect optic nerve damage and assess intraocular pressure14 17. The disease is characterized by progressive loss of retinal ganglion cells and thinning of the retinal nerve fiber layer, which can be detected with imaging technologies7 18.
Key diagnostic tools include:
- Tonometry: Measures intraocular pressure, a critical parameter since elevated IOP is a major risk factor17 12.
- Gonioscopy: Examines the anterior chamber angle to differentiate open-angle from angle-closure glaucoma17 .
- Optical Coherence Tomography (OCT): Provides detailed imaging of the retinal nerve fiber layer to detect glaucomatous damage18 .
- Dilated Fundus Examination: Assesses the optic nerve head for characteristic glaucomatous changes such as increased cup-to-disc ratio17 4.
- Visual Field Testing: Detects peripheral vision loss and monitors disease progression17 .
- Corneal Thickness Measurement: Helps interpret IOP readings accurately, as corneal thickness can affect pressure measurements17 .
- Slit Lamp Biomicroscopy: Evaluates the anterior segment and optic nerve head17 .
Diagnosis also requires excluding other optic nerve and retinal diseases or neurological disorders that may mimic glaucoma14 .
Stages of Open-Angle Glaucoma
Glaucoma staging is based on the severity of optic nerve damage and visual field loss17 4. The disease progresses through the following stages:
| Stage | Characteristics | Visual Field Impact |
|---|---|---|
| Early | Minimal optic nerve damage; no or subtle visual field loss | Often asymptomatic; peripheral vision intact |
| Moderate | Noticeable optic nerve changes; visual field defects appear | Peripheral vision loss begins; scotomas develop |
| Advanced | Significant optic nerve damage; extensive visual field loss | Tunnel vision; central vision usually preserved |
| End-stage | Severe optic nerve damage; near-total visual field loss | Central vision affected; risk of blindness |
| Sources: 174 | ||
Early detection and treatment are essential to slow progression and preserve vision19 4.
Glaucoma is a unique optic neuropathy characterized by damage to the optic nerve. Structure and function are complementary in glaucoma diagnosis13 .
Open-Angle Glaucoma Treatment Options
The primary goal of treatment is to lower intraocular pressure to prevent further optic nerve damage and slow disease progression8 4. Treatment options include medicated eye drops, oral medications, laser therapy, and surgery.
Medicated Eye Drops
Topical medications are the first-line treatment for open-angle glaucoma20 . They work by either increasing aqueous humor outflow or decreasing its production to reduce IOP.
Common classes of eye drops include:
- Prostaglandin analogs: Increase aqueous humor outflow through the uveoscleral pathway; commonly prescribed due to efficacy and once-daily dosing20 .
- Beta-blockers: Decrease aqueous humor production; often used in combination with other agents20 .
- Adrenergic agonists: Reduce aqueous humor production and increase outflow20 .
- Carbonic anhydrase inhibitors: Reduce aqueous humor secretion; available as topical agents20 .
Adherence to eye drop therapy is critical but often poor, with many patients discontinuing treatment early13 21.
Oral Medications
Oral carbonic anhydrase inhibitors, such as acetazolamide, are used for acute or refractory glaucoma cases when rapid IOP reduction is needed20 . Mannitol, an osmotic agent, may also be used to quickly lower eye pressure in emergencies20 .
Laser Therapy
Laser treatments improve aqueous humor outflow by targeting the trabecular meshwork or reducing aqueous humor production22 .
- Laser trabeculoplasty: Enhances drainage through the trabecular meshwork and is effective in lowering IOP22 .
- Cyclophotocoagulation: Reduces aqueous humor production by targeting the ciliary body22 .
Selective laser trabeculoplasty can be considered as a first-line therapy, especially for patients with poor medication adherence13 .
Surgery
Surgical options are reserved for patients who do not respond adequately to medications or laser therapy. Procedures aim to create new drainage pathways or implant devices to lower IOP8 20.
Medication adherence is a significant challenge in glaucoma care, with up to 70% of doses missed in some studies13 .
Preventing Open-Angle Glaucoma
While primary open-angle glaucoma cannot be fully prevented, early detection and treatment are essential to manage the disease and prevent vision loss19 . Regular comprehensive eye exams starting at age 40 are recommended, with increased screening frequency for individuals with risk factors such as family history or African descent14 17.
Prevention strategies focus on:
- Regular eye examinations to detect glaucoma before symptoms appear17 .
- Controlling intraocular pressure through prescribed medications or procedures8 .
- Educating patients on the importance of medication adherence and follow-up care19 .
- Protecting eyes from injury and managing systemic conditions that may increase risk16 .
Conditions Related to Open-Angle Glaucoma
Open-angle glaucoma is part of a group of optic neuropathies that cause progressive vision loss. Related conditions include:
- Normal-tension glaucoma: Optic nerve damage occurs despite normal IOP, possibly due to optic nerve sensitivity or reduced blood flow16 3.
- Neovascular glaucoma: A painful secondary glaucoma caused by retinal vein occlusion or other ischemic eye diseases, leading to new blood vessel growth that blocks aqueous outflow14 .
- Secondary open-angle glaucoma: Caused by other conditions that clog the drainage system, such as pigment dispersion or trauma3 .
Timely diagnosis and treatment of these related conditions are crucial to prevent severe vision loss19 .
Living With Open-Angle Glaucoma
Living with open-angle glaucoma requires ongoing management to slow disease progression and preserve remaining vision. Untreated glaucoma can lead to severe vision impairment, tunnel vision, and ultimately complete blindness2 7. The disease affects daily activities and quality of life, making support and adaptive strategies important24 .
Vision loss from glaucoma cannot be reversed, but early diagnosis and consistent treatment can slow progression and preserve sight19 2.
Patients can benefit from:
- Improving lighting conditions to aid vision24 .
- Using assistive devices such as magnifiers to compensate for vision loss24 .
- Seeking social support and joining peer or advocacy groups for emotional and practical assistance24 .
Regular follow-up with eye care professionals and adherence to treatment are essential to maintain vision and quality of life19 3.