Glaucoma affects over 70 million people worldwide and is a leading cause of irreversible blindness, especially in older adults1 . This group of eye diseases damages the optic nerve, often silently, until vision loss occurs2 . Early detection through comprehensive eye exams and specialized tests is crucial to prevent or slow down permanent vision loss3 4. Understanding the diagnostic process helps patients and clinicians identify glaucoma early and manage it effectively5 .
Medical History and Symptoms
A thorough medical history is the first step in glaucoma diagnosis. Eye care professionals inquire about symptoms, family history, and medication use to assess risk3 . Glaucoma often has no symptoms in its early stages, making history-taking vital3 . When symptoms do appear, they may include blurry vision, eye pain, or headaches6 . A family history of glaucoma significantly increases risk, as does long-term corticosteroid use3 6.
Other medical conditions such as diabetes, hypertension, coronary heart disease, and smoking are linked to higher glaucoma risk or refractory glaucoma (glaucoma resistant to treatment) 73. Age is a major factor; glaucoma prevalence rises with age, reaching about 10% in people over 90 years old4 . Certain ethnic groups, including African, Hispanic, and Asian populations, also have higher risks8 .
- Key risk factors assessed during history taking include:
- Age over 40 years8
- Family history of glaucoma3
- Diabetes and hypertension7
- Long-term steroid medication use6
- Smoking and cardiovascular disease7
“Glaucoma is a disease that damages your eye's optic nerve. It usually happens when fluid builds up in the front part of your eye. That extra fluid increases the pressure in your eye, damaging the optic nerve.”
— J. Kevin McKinney, American Academy of Ophthalmology9
Eye Pressure Measurement (Tonometry)
Tonometry measures the intraocular pressure (IOP), the fluid pressure inside the eye, which is a key factor in glaucoma diagnosis and management3 . Elevated IOP can damage the optic nerve, but normal IOP does not rule out glaucoma, as some patients develop glaucoma with pressures within the normal range (10–21 mmHg) 35.
Several tonometry methods exist:
- Goldmann Applanation Tonometry: The gold standard, it measures the force needed to flatten a small area of the cornea after numbing the eye with anesthetic drops3 10.
- Electronic Indentation Tonometry: A portable device that touches the cornea and instantly records IOP3 .
- Non-Contact Tonometry: Uses a puff of air to flatten the cornea and measure pressure without touching the eye3 10.
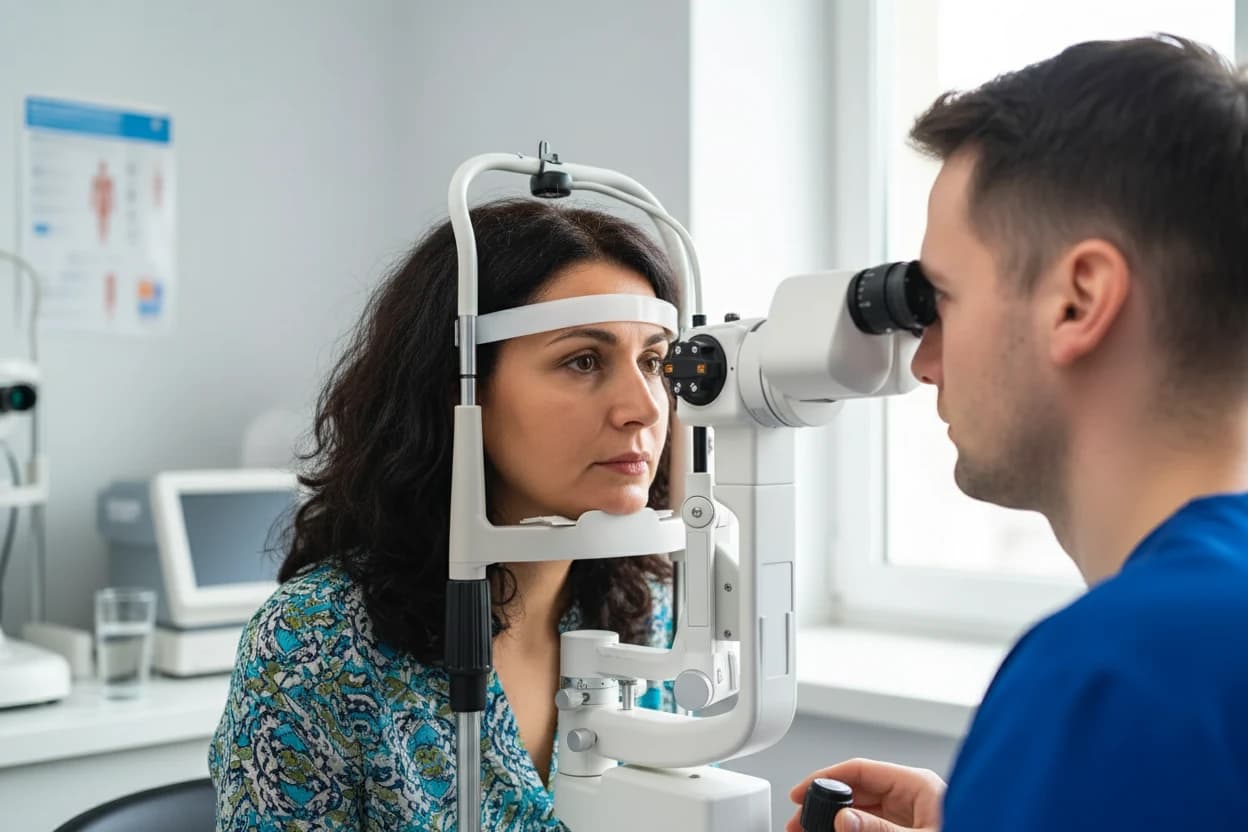
During the test, the patient rests their chin and forehead on a support to keep the head steady10 . The test is painless, though the air puff may cause mild pressure sensation10 . Corneal thickness affects tonometry readings, so pachymetry is often performed to adjust measurements3 .
Tonometry is also used to monitor treatment effectiveness in glaucoma patients11 . Elevated IOP requires close follow-up and often treatment to prevent optic nerve damage5 .
- Important facts about tonometry:
- Normal IOP range: 10–21 mmHg3
- Some glaucoma patients have normal IOP (normal-tension glaucoma) 3
- Corneal thickness influences IOP measurement accuracy3
- Eye drops are used to numb the eye before contact tonometry3 10
- Regular tonometry helps monitor glaucoma progression and treatment11
Tonometry refers to a type of eye test that measures pressure inside your eye (intraocular pressure). It's one of the essential glaucoma tests.
Corneal Thickness Test (Pachymetry)
Pachymetry measures the thickness of the cornea, the clear front layer of the eye, which influences the accuracy of intraocular pressure readings3 . A thin cornea can lead to underestimation of IOP, potentially delaying glaucoma diagnosis3 4. Conversely, a thicker cornea may cause overestimation.
The test uses a small probe that gently touches the cornea after numbing drops are applied3 . Results from pachymetry help eye care professionals adjust IOP measurements and assess glaucoma risk more accurately3 .
- Key points about pachymetry:
- Measures corneal thickness to improve IOP accuracy3
- Thin cornea is a recognized risk factor for glaucoma3
- Helps adjust tonometry results for better diagnosis3
- Quick and painless procedure with a small probe3
Visual Field Testing (Perimetry)
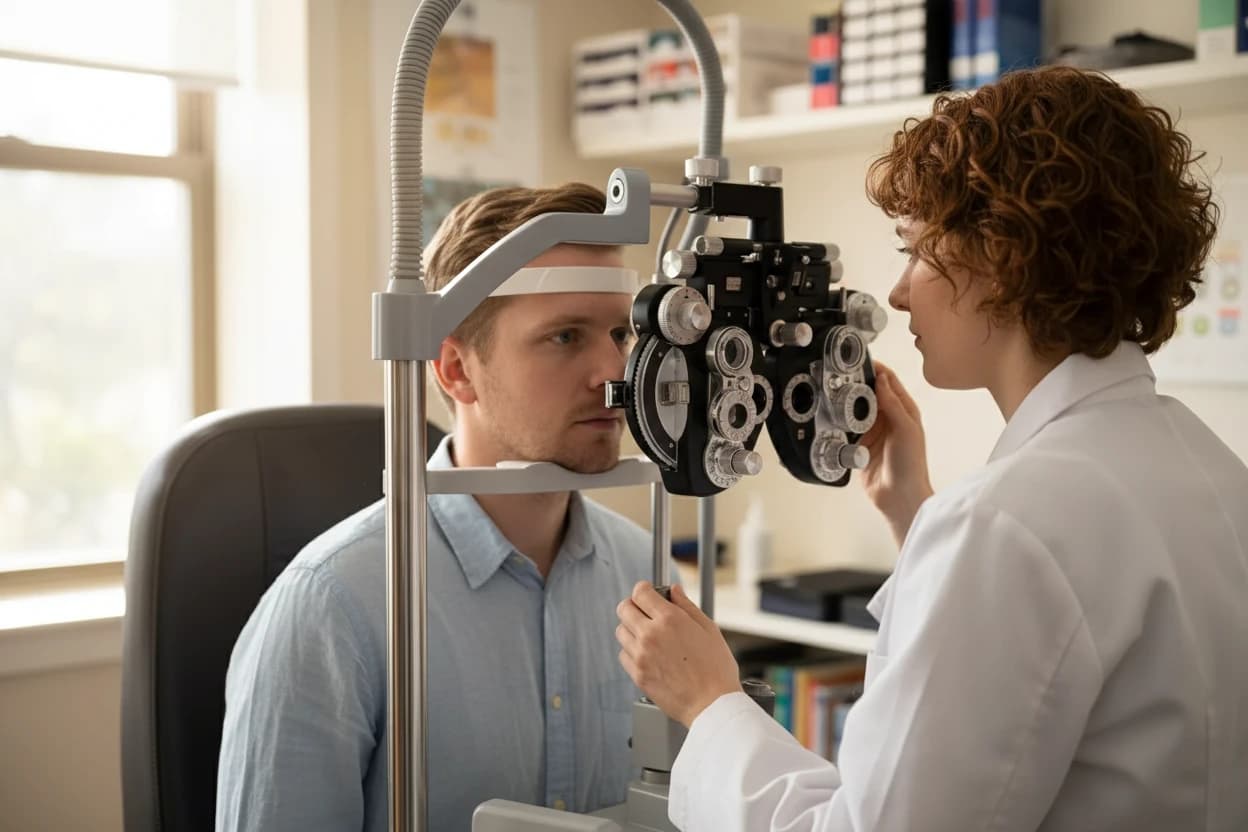
Visual field testing, or perimetry, evaluates peripheral (side) vision, which is often affected early in glaucoma3 . This test detects vision loss before patients notice symptoms3 4. It is performed using a perimeter, a bowl-shaped instrument that flashes small lights in different areas of the visual field3 .
Each eye is tested separately, and lenses may be used to correct vision during the test3 . The patient presses a button when they see a light, allowing the machine to map the visual field3 . Results are compared to normal charts to identify areas of vision loss and determine glaucoma severity3 .
- Visual field testing features:
- Detects peripheral vision loss characteristic of glaucoma3
- Uses a bowl-shaped perimeter device3
- Tests each eye individually3
- Patient responds to light stimuli by pressing a button3
- Helps monitor disease progression over time3
Visual field testing is critical because glaucoma often damages peripheral vision first. Early detection through perimetry can prevent unnoticed vision loss and guide timely treatment. 34
Retina and Optic Nerve Examination
Ophthalmoscopy (also called funduscopy) allows direct visualization of the optic nerve at the back of the eye3 . This examination is essential for detecting glaucomatous damage, such as optic nerve cupping, where the central depression of the nerve enlarges due to nerve fiber loss3 4.
The test is performed after dilating the pupil with eye drops to improve visibility3 . Using an ophthalmoscope, the eye care professional assesses the optic nerve for signs of damage and compares findings over time3 .
- Key aspects of ophthalmoscopy:
- Directly examines the optic nerve for glaucoma signs3
- Pupil dilation enhances visualization3
- Detects optic nerve cupping, a hallmark of glaucoma3
- Helps differentiate glaucoma from other optic nerve diseases3
Optic Nerve Imaging (OCT)
Optical Coherence Tomography (OCT) is a non-invasive imaging technique that provides detailed cross-sectional images of the retina and optic nerve3 4. OCT detects structural changes in the optic nerve and retinal nerve fiber layer before vision loss occurs, making it valuable for early diagnosis and monitoring3 .
During the test, the patient sits comfortably with their head supported while light waves scan the eye3 . OCT can track disease progression and assess treatment response by measuring nerve fiber thickness over time3 .
- Benefits of OCT in glaucoma diagnosis:
- Provides high-resolution images of optic nerve and retina3
- Detects early structural damage before visual field loss3
- Non-invasive and quick procedure3
- Useful for monitoring disease progression and treatment efficacy3
OCT is a powerful tool that reveals subtle optic nerve damage invisible to standard eye exams, enabling earlier intervention to protect vision. 34
Drainage Angle Assessment (Gonioscopy)
Gonioscopy examines the drainage angle of the eye, where aqueous humor fluid exits to maintain healthy eye pressure3 . A narrow or blocked drainage angle is a significant risk factor for glaucoma, especially angle-closure glaucoma3 4.
The procedure involves numbing the eye with drops and placing a special handheld lens on the eye to visualize the angle using a slit lamp microscope3 . This test helps distinguish between open-angle and angle-closure glaucoma, guiding appropriate treatment3 .
- Important points about gonioscopy:
- Examines the eye’s drainage angle to assess fluid outflow3
- Performed after numbing the eye with anesthetic drops3
- Uses a handheld lens and slit lamp for visualization3
- Identifies narrow or blocked angles that increase glaucoma risk3
- Essential for diagnosing angle-closure glaucoma3
Glaucoma is an umbrella term for eye diseases that make pressure build up inside your eyeball, which can damage delicate, critical parts at the back of your eye.
Diagnosis Process Summary
Diagnosing glaucoma requires a comprehensive approach combining history, clinical examination, and specialized tests3 4. No single test confirms glaucoma; instead, diagnosis is based on a combination of findings over time5 .
Typical diagnostic steps include:
- Reviewing medical history and risk factors3
- Measuring intraocular pressure with tonometry3
- Assessing corneal thickness with pachymetry to adjust IOP readings3
- Testing peripheral vision with visual field testing (perimetry) 3
- Examining the optic nerve via ophthalmoscopy after pupil dilation3
- Imaging the optic nerve and retina using OCT for early structural changes3
- Inspecting the drainage angle with gonioscopy to classify glaucoma type3
Glaucoma is often asymptomatic until advanced stages, so regular comprehensive eye exams are crucial for early detection and management3 4. Early diagnosis allows for treatment to lower eye pressure and prevent further optic nerve damage5 .
| Diagnostic Test | Purpose | Key Outcome |
|---|---|---|
| Medical History | Identify risk factors and symptoms | Risk stratification |
| Tonometry | Measure intraocular pressure (IOP) | Detect elevated eye pressure |
| Pachymetry | Measure corneal thickness | Adjust IOP measurements |
| Visual Field Testing | Assess peripheral vision loss | Detect functional vision defects |
| Ophthalmoscopy | Examine optic nerve for damage | Identify optic nerve cupping |
| Optical Coherence Tomography (OCT) | Image optic nerve and retinal layers | Detect early structural changes |
| Gonioscopy | Inspect eye drainage angle | Determine glaucoma type |
| Sources: 1234567891011 | ||